Department of Pathology Updates - Vol 2.2
By Jeffrey Myers | December 20 2016Teammates and colleagues,
Welcome to a frigid edition of DOP Updates, an email sent to members of our Department of Pathology (DOP) to spark conversations around strategic goals, our brand, and the things that matter most. Updates is also attached as a PDF to overcome any formatting defects that may occur on whatever the mobile device you may be using to read it. Updates is sent with a strong belief that why we do what we do supersedes what we do and how we do it when it comes to purpose and making a difference in the lives of one another and those we serve.
Marching (April 22, 2016)
No taller than 4 feet for certain; even that might be a stretch. Marching along the hospital corridor flooded by a lunch time crowd, her measured stride making nearly as much progress side-to-side as it did forward. She paid little attention to the giants who flowed around her. They in turn paid little attention to her while effortlessly avoiding her wake.
Her little arms pumped rhythmically to a drummer that only she could hear, each step closer to a place unknown. What remained of her hair stuck out above the straps that kept a mask affixed to her face with only her deep brown eyes to convey the fear that lingered at the corners. Her gay colored pink and blue dress advertised a determination to be normal; to be like other little girls for whom this was a time of wonder rather than a time of worry.
Her mother walked less confidently behind, just off the beat as she followed single file with her stare fixed firmly on her phone oblivious to the course being plotted in front of her.
I said a prayer, hopeful that her daughter would take her to a place of unanticipated joy while silently wishing for them to be happy.
Patient and Family Centered Care (PFCC) comes to pathology
Since last summer we have been making substantial investments in patient and family centered care (PFCC), a suite of methodologies that Don Berwick (pediatrician, President Emeritus and Senior Fellow at the Institute for Healthcare Improvement (IHI), former Administrator of the Centers for Medicare & Medicaid Services, and long time faculty member of Harvard Medical School and Harvard School of Public Health) describes as, “The most direct route to the Triple Aim.” The Triple Aim is an IHI framework for optimizing the performance of health systems and comprises three elements:
- improving the patient experience of care,
- improving the health of populations, and
- reducing the cost of care.
PFCC is not care as we’ve traditionally provided it. It shares the same commitment to patients and their welfare that has always driven the best of medicine, past, present and future, whether it be the care we deliver today, educating those who will care for us, or pushing the boundaries of knowledge and technology to create health care of the sort that we can only dream of today. And while what we’ve always done to and for patients speaks to the very best of intentions, PFCC differs in focusing on the importance of working with patients and their families to build mutually beneficial partnerships in which value is understood from the perspective of those entrusted to our care rather than the other way ‘round. PFCC is framed by core principles that include dignity and respect, sharing information that is affirming and useful, participation, and collaboration.
In July with the help of Molly White and Kate Balzer (manager and project manager, respectively, for our UMHS adult PFCC program) we launched what may be the first pathology-based Patients and Families Advisory Council (PFAC). Our PFAC was created to understand and implement strategies that bring us closer to a place in which PFCC forms the very foundation of our work. Our PFAC currently stands at 40 members including 7 Patient and Family Advisors (PFAs). PFAs are UMHS patients and family members, vetted and trained by our UMHS PFCC staff, who volunteer time and energy to help us do better tomorrow what we may already do well today. They help us identify and understand those things that already work well, while also helping us to see important opportunities for continuous improvement. The remainder of our PFAC comprises staff, trainees and faculty from our divisions of anatomic pathology (AP), clinical pathology (CP), experimental pathology (EP), MLabs, pathology informatics (PI), and quality and health improvement (DQHI).
Our PFAC is much bigger than the usually recommended size, but is appropriate to the task at hand which includes transforming our culture that we might understand the power of working directly with patients and their families rather than continuing to operate behind a semi-opaque veil that separates those we serve from the expertise important to fully understanding actionable information that drives so much of the decision making that shapes their health care journeys. Through a series of brainstorming exercises we have chosen as our current areas of focus,
- sharing the information generated in our laboratories with patients and families in ways that are affirming and useful,
- creating opportunities for patients and families to more effectively understand and participate in application of pathology to their health care journeys, and
- identifying ways to stand alongside patients and families to build mutually beneficial partnerships of value that narrow the gap between the health care they receive today and the care to which they are entitled.
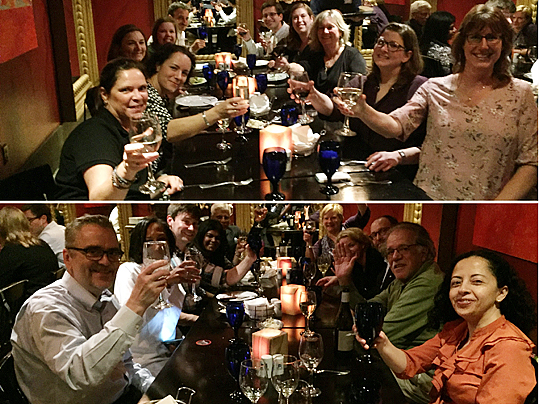 Last month a large team of 21 PFAC members, including 3 PFAs, traveled to an intensive training seminar offered by the Institute for Patient and Family Centered Care (IPFCC) in San Antonio, Texas. We were the single largest team in attendance; never before in their history had they hosted a pathology-based team! Can’t think of a department better positioned to demonstrate the rewards realized from working directly with patients and families to achieve excellence in all that we do. Over a period of 2.5 days we spread ourselves across the program to take advantage of every opportunity to learn more about the importance of mutually beneficial partnerships with patients and their families as a strategy for improving the experience of care and addressing challenges in patient safety and the cost of the services we deliver. We saw the power of patient stories to galvanize our common purpose, reminding us why we do what we do every day and the satisfaction of achieving great! rather than the merely good. We were reminded that our frontline champions are not in our conference rooms or boardrooms but at the bench, in our labs, in our signout rooms, and in the places common to the work that touches the lives of the thousands of patients who travel through our laboratories every week. We learned that our patients define who is family to them, people to whom they are related in any way whether it be biologically, legally or emotionally. We learned that there are countless barriers, erected with the very best of intentions, that stand between our patients and the care that they and their families deserve.
Last month a large team of 21 PFAC members, including 3 PFAs, traveled to an intensive training seminar offered by the Institute for Patient and Family Centered Care (IPFCC) in San Antonio, Texas. We were the single largest team in attendance; never before in their history had they hosted a pathology-based team! Can’t think of a department better positioned to demonstrate the rewards realized from working directly with patients and families to achieve excellence in all that we do. Over a period of 2.5 days we spread ourselves across the program to take advantage of every opportunity to learn more about the importance of mutually beneficial partnerships with patients and their families as a strategy for improving the experience of care and addressing challenges in patient safety and the cost of the services we deliver. We saw the power of patient stories to galvanize our common purpose, reminding us why we do what we do every day and the satisfaction of achieving great! rather than the merely good. We were reminded that our frontline champions are not in our conference rooms or boardrooms but at the bench, in our labs, in our signout rooms, and in the places common to the work that touches the lives of the thousands of patients who travel through our laboratories every week. We learned that our patients define who is family to them, people to whom they are related in any way whether it be biologically, legally or emotionally. We learned that there are countless barriers, erected with the very best of intentions, that stand between our patients and the care that they and their families deserve.
Our PFAC is currently engaged in a process to,
1) extend the experience to all PFAC members in a manner that allows equal footing and participation in the conversation going forward,
2) do a simple gap analysis ("gut check") to measure our current state against what we learned regarding PFCC principles and methodologies, and
3) develop and implement a tactical plan and achievable projects focused on the thematic areas outlined above.
Other work that quickly followed our return from San Antonio includes exploratory conversations with organizations outside of our own to understand how we can do a better job of hearing our own stories from UMHS and MLabs patients and families touched by the work that we do. If YOU have a story that you would like to contribute to our archive please send me a note. It is our hope that in the next few months we can adopt as standard practice opening many of our meetings (e.g., QA meeting, meetings of our various operations groups, faculty meetings, LCC) with stories that remind us our common purpose whether it be in the care that we provide today, our educational programs, or our commitment to create the future of health care through discovery and innovation. We have also identified opportunities for PFAs to work with us more directly, including pathology-based committees both local and national and detailed design of patient care areas relevant to PRR.
Please join me in CONGRATULATING our PFAC members, including especially our 7 PFAs, on the great work that they are doing to make pathology at UMHS (soon to be Michigan Medicine) a leader in understanding how PFCC applies to the work that we do.
HAPPY HOLIDAYS!
Let me end by THANKING each and every one of you for the countless things you do to remind us why we are here, and how our work matters in a world much bigger than we are. Whatever your background, culture, country of origin, political affiliations, or religious beliefs, this is a special time of year for reasons that go well beyond traditionally celebrated holidays. It is the end of another year complete with seasonal shifts that bring snow to our roads, frost to our windows, and color to our cheeks. It is a time to reflect on the personal challenges that you leave behind and those that you have yet to face, the challenges that we confront together, and the blessings that make ours a place of privilege in a world too often divided. It is a time to reflect on our fellow human beings who are cold, hungry, lonely, and afraid. It is a time to celebrate our shared humanity with determination that the things that bind us are stronger than the forces pushing us apart. It is a time to be reminded that kindness is a useful and important strategy for those with the courage to believe that 2017 will prove to be a year of wonder, healing, and opportunity.
However you choose to celebrate this special time of year, may the time you spend with friends and family be nourishing in ways that go well beyond the dinner table, and may the New Year bring you unanticipated moments of joy.
Happy New Year.
 ON THE COVER
ON THE COVER
 ON THE COVER
ON THE COVER
 ON THE COVER
ON THE COVER
 ON THE COVER
ON THE COVER
 ON THE COVER
ON THE COVER
 ON THE COVER
ON THE COVER
 ON THE COVER
ON THE COVER
 ON THE COVER
ON THE COVER
 ON THE COVER
ON THE COVER
 ON THE COVER
ON THE COVER
 ON THE COVER
ON THE COVER
